- Home
- Clinician Area
- COVID-SURG CANCER
Study Reveals Low Risk of COVID-19 Infection Among Patients Undergoing Head and Neck Cancer Surgery
COVIDSurg Collaborative. CANCER; Published Online: December 21, 2020 (DOI: 10.1002/cncr.33320).
http://doi.wiley.com/10.1002/cncr.33320
 A recent international observational study provides important data on the safety of head and neck cancer surgery during the COVID-19 pandemic. The findings are published online in CANCER, The study is part of the COVIDSurg Collaborative, an initiative to describe surgical practices during the early period of the pandemic, when many hospitals had limited capacity and when it was unclear whether it was safer to delay or continue in-hospital cancer treatments.
A recent international observational study provides important data on the safety of head and neck cancer surgery during the COVID-19 pandemic. The findings are published online in CANCER, The study is part of the COVIDSurg Collaborative, an initiative to describe surgical practices during the early period of the pandemic, when many hospitals had limited capacity and when it was unclear whether it was safer to delay or continue in-hospital cancer treatments.
The early consensus was that head and neck surgery was very risky for patients, and the treating surgeon. There was a concern regarding less fit or elderly patients, or those who required complex procedures or reconstructive surgery and the risk to the treating surgeon due to AGPs.
The data in this study is reassuring in regard to the risk to patients, showing that with appropriate precautions there is no additional risk of COVID-19 for these groups. The findings emphasise the importance of following the correct procedures for staff, in particular with regard to tracheostomies.
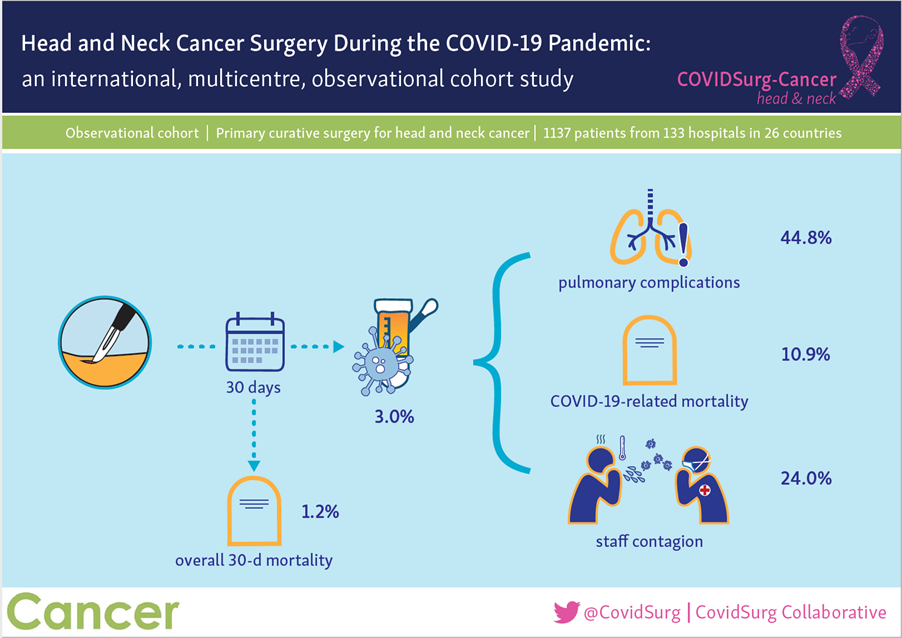
The COVIDSurg Collaborative examined information on 1,137 patients with head and neck cancer undergoing potentially curative surgery in 26 countries. The most common sites were the oral cavity (38 percent) and the thyroid (21 percent). The death rate within 30 days after surgery was 1.2 percent, a rate that would be normally expected in this patient population, without a pandemic. Also, 29 (3 percent) patients tested positive for COVID-19 within 30 days of surgery; of these 13 (44.8 percent) developed severe respiratory complications and three (10.9 percent) died – representing serious consequences. Clinicians now know that these risks can be minimized with precautions such as staff testing, infection control measures and vaccination.
Patients were more likely to test positive for COVID-19 when they lived in communities with high levels of COVID-19, when they had oral tumors, and when they received a tracheostomy (an opening created in the neck to facilitate placing a tube into the windpipe).
BAHNO has been at the forefront of supporting this work and with the continued support of the membership will be following up the cohort going forward.
Corresponding author Richard J. Shaw, Liverpool Head & Neck Centre, University of Liverpool
International Cancer Leads Stuart Winter, Consultant ENT Surgeon, Oxford, Andrew G Schache Consultant OMFS Surgeon, Liverpool